

Hier erfährst du, was in deinem Körper im Zyklus passiert und woran du erkennst, ob er gesund ist.
Cycle health describes the state in which the body’s hormonal processes work together harmoniously. “Healthy” here means that the female cycle follows a biologically meaningful pattern—i.e., it is fairly regular, stable and includes fertile days.
Important: A healthy cycle is not a rigid construct of exactly 28 days, but an individual rhythm that—depending on your cycle type—moves within a certain range and reliably produces ovulation. What matters is not the perfect length, but functionality: ovulation occurs, hormones rise and fall at the right time, and your period follows as the natural end of the luteal phase. A stable cycle has a positive effect on energy levels, mood, sleep quality, metabolism and fertility.
Factors such as stress, diet, sleep or illness can disrupt this sensitive process. Cycle health therefore also means understanding the processes in your own body and recognizing early when hormonal patterns are getting out of balance. Modern cycle diagnostics—such as continuous core body temperature measurement with OvulaRing—makes it possible to objectively visualize your cycle health and classify individual changes in an understandable way.
A healthy menstrual cycle is the result of a finely tuned interplay between the brain, hormones, ovaries and uterus. At the center is ovulation—because it determines whether the cycle is fertile and whether the hormonal phases run stably. A cycle usually consists of two main phases (follicular phase and luteal phase) and four characteristic sections, which differ in temperature, hormones and physical changes.
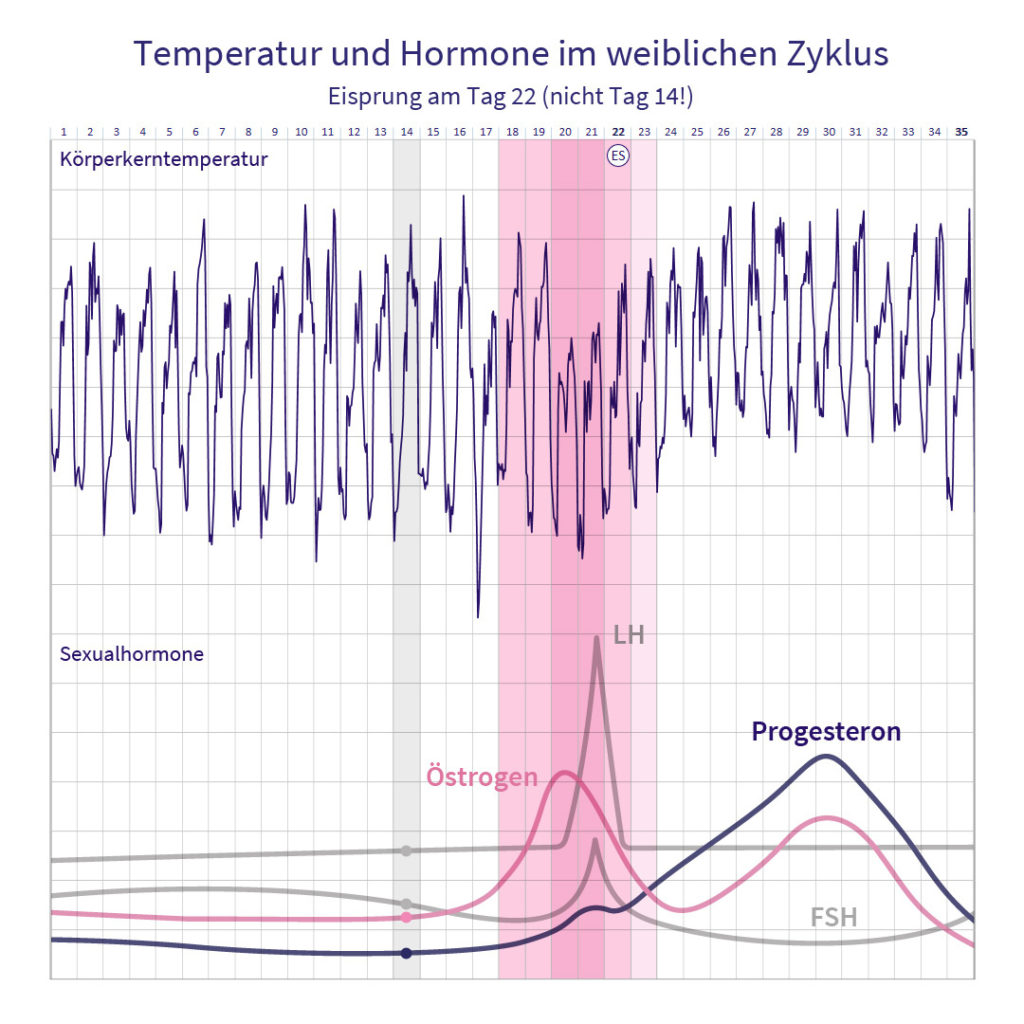
A healthy cycle (a biphasic cycle with 2 pronounced main phases) is divided into four repeating sections:
These four phases ensure that the cycle fulfills its biological purpose: enabling ovulation and preparing for implantation of a fertilized egg.
In the ovaries, follicle growth and ovulation control the hormonal course of the entire cycle. During the follicular phase, several follicles mature until a dominant follicle is selected. This follicle produces increasing amounts of estrogen and signals to the brain that an egg will soon be ready.
At ovulation, a strong LH surge (the so‑called LH peak) triggers the rupture of the dominant follicle. After the egg is released, the follicle becomes the corpus luteum, which produces progesterone—a hormone that is important for a stable luteal phase.
Disruptions in these processes can mean that ovulation does not occur or happens too late, which is common with PCOS or stress-related strain.
In parallel with the hormonal changes in the ovaries, the uterine lining builds up rhythmically:
This regular build-up and breakdown of the lining is an indication of a functioning hormonal balance.
Ovulation is the most important indicator of a healthy cycle. Only when ovulation takes place does the cycle run its full course and remain hormonally balanced. It determines:

A missing ovulation means that no (or too little) progesterone is produced – the luteal phase becomes unstable or is completely absent. This often leads to long cycles, spotting or an unfulfilled desire to have a child.
With cycle data such as continuous temperature measurement, you can determine whether and when ovulation occurred—much more precisely than by noting symptoms or using apps.
Several hormones control the monthly cycle. The most important are:
A balanced interplay of these hormones ensures stable cycles. Deviations—such as low progesterone levels, elevated LH levels (typical in PCOS) or impaired estrogen production—can significantly affect the cycle.
A healthy cycle is not only reflected by its length, but by the harmonious interaction of different hormonal and physical signals. What matters is that the cycle is functional—i.e., it produces ovulation regularly and shows stable hormone patterns. A healthy cycle supports physical and emotional well-being, has a positive effect on energy levels and metabolism, and is a key indicator of overall hormonal health.
A healthy cycle typically lasts between 21 and 35 days. The length may vary as long as fluctuations remain moderate—around up to 7–10 days. So what matters is not the exact number, but relative stability. Strong or sudden changes can indicate hormonal imbalances, for example due to stress, thyroid changes or PCOS (polycystic ovary syndrome). Regular cycles suggest that ovulation occurs reliably and that hormonal communication between the brain and ovaries works well.
Ovulation is the heart of cycle health. A stable ovulation that occurs in every cycle shows that the body produces enough progesterone, follicle maturation works and the luteal phase fulfills its role. Typical signs of ovulation include a clear temperature rise after ovulation, changes in cervical mucus and, for some women, a slight pulling sensation in the lower abdomen. If ovulation does not occur, the cycle is hormonally incomplete—common consequences are long cycles, PMS-like symptoms or difficulties when trying to conceive.
A healthy period usually lasts 3–7 days and has a consistent intensity that is neither excessively heavy nor unusually light. Signs of balanced bleeding include: neither extremely heavy nor noticeably light, little to moderate pain and a limited duration without prolonged spotting. Heavy bleeding can indicate fibroids, endometriosis, a disturbed lining or thyroid problems. Very light bleeding or so‑called “withdrawal bleeding” (without ovulation) often occurs with anovulation (a cycle without ovulation), PCOS or hormonal imbalance.
A hormonally healthy cycle is accompanied by cyclical but stable changes in energy, mood and resilience. Typical patterns of a balanced cycle are: more energy and focus in the follicular phase, a calmer body feeling in the luteal phase, and mild mood swings before your period. Extreme performance drops or strong emotional episodes, on the other hand, can indicate hormonal disorders, for example PMDD, low progesterone or chronic stress.
The menstrual cycle influences numerous bodily systems. A healthy cycle can have a positive effect on the skin (less inflammatory acne), sleep (more restful, especially in the follicular phase) and metabolism (natural but not extreme fluctuations in appetite and energy). Changes in these areas can indicate hormonal imbalances—common causes include progesterone deficiency (luteal phase defect), thyroid disorders, PCOS or chronic stress.
Cycle health disorders are common and can have very different causes. They can be temporary and harmless or indicate hormonal imbalances and medical conditions. Typical cycle irregularities and cycle disorders affect cycle length, the strength or type of bleeding and whether ovulation has occurred. Many of these changes can be influenced by lifestyle factors such as stress, lack of sleep or diet; others require medical evaluation.
Cycles are considered irregular when cycle length varies greatly from month to month or the intervals between periods differ significantly. Fluctuations of more than 7–10 days are a clear sign of hormonal instability. Common reasons include stress, lack of sleep, thyroid disease, major weight changes or PCOS. Irregular cycles usually occur because ovulation is delayed or does not happen at all.
Cycles longer than 35 days are referred to as oligomenorrhea (long cycle). They often result from delayed ovulation or absent ovulation (anovulation). The body may then try for weeks to trigger ovulation, unnecessarily prolonging the follicular phase. Common causes include PCOS, stress, an underactive thyroid, the hormonal transition after stopping the pill or being underweight. With long cycles, a stable progesterone rise is often missing, which can lead to PMS, spotting or an unfulfilled desire to have a child.
Short cycles under 21 days can indicate that the follicular phase is shortened or the luteal phase is too short. Luteal phases that are too short are often caused by low progesterone levels after ovulation and can reduce the likelihood of successful implantation. Hormonal contraception during the discontinuation phase, stress or the beginning of perimenopause can also cause short cycles.
Anovulation means that no ovulation occurs in a cycle. As a result, no progesterone is produced—the cycle remains hormonally incomplete. Typical symptoms include long cycles, unclear temperature curves, intermenstrual bleeding and mood swings. Common causes include PCOS, intense training, chronic stress, being significantly under- or overweight, and thyroid disorders. Anovulatory cycles are also common immediately after stopping the pill.
Strong temperature fluctuations or unclear patterns can indicate hormonal instability, irregular ovulation or disturbances of the luteal phase. While an elevated baseline temperature after ovulation is normal, constantly changing or flat curves are often a sign of insufficient progesterone production. Lack of sleep, alcohol or shift work also influence temperature patterns. Continuous temperature measurement allows these patterns to be recognized much more precisely than once‑daily measurement.
PMS (premenstrual syndrome) includes physical and psychological symptoms before your period that are triggered by the hormone drop at the end of the cycle. Typical symptoms include irritability, breast tenderness, water retention, fatigue and mood swings. PMDD (premenstrual dysphoric disorder) is a rarer, significantly more severe form that can cause pronounced emotional distress. Progesterone deficiency, stress, sleep problems or neuroendocrine sensitivity are often underlying factors.
Spotting is light, brownish or bright‑red bleeding outside the regular period. It can be harmless—for example around the time of ovulation or at the beginning of the luteal phase—or it can indicate hormonal disturbances. Common causes include progesterone deficiency, absent ovulation, changes in the lining, thyroid problems, PCOS or the influence of hormonal contraception. Cycles immediately after stopping the pill are also often accompanied by spotting.
Further information: Main article on cycle disorders
Cycle problems arise when the finely tuned interplay of hormones, brain, metabolism and lifestyle gets out of balance. Many factors can influence the cycle—some short term, others long term. The most common causes include stress (physical or emotional), diet, the thyroid, PCOS, hormonal contraception, chronic conditions and sleep rhythms. Understanding these triggers helps you classify cycle changes better and improve them in a targeted way.
Stress is one of the most common causes of irregular or prolonged cycles. Under strain, the body releases more cortisol, which can inhibit the release of GnRH, FSH and LH—hormones responsible for triggering ovulation. Persistent mental stress, overload, emotional strain or lack of sleep often delay follicle maturation or prevent it altogether. Typical result: long cycles, delayed ovulation or anovulatory cycles.
A balanced diet and stable energy intake are crucial for cycle health. Large calorie deficits, being underweight, extreme diets or intensive athletic strain can lead to hormonal disruptions because the body switches into “energy‑saving mode”. Certain nutrient deficiencies (e.g., iron, vitamin D, omega‑3 fatty acids or B vitamins) also affect hormone production, thyroid function and metabolism. The cycle reacts sensitively to under- or overnutrition—often with long or absent cycles. More info here: Nutrition across the cycle
The thyroid plays a central role in hormone and metabolic balance. Both an underactive thyroid (hypothyroidism) and an overactive thyroid (hyperthyroidism) can cause cycle problems. With hypothyroidism, long cycles, heavier bleeding, fatigue and weight gain are common. Hyperthyroidism more often leads to short cycles, nervousness and weight loss. Thyroid hormones act directly on ovarian activity, so even slight changes can trigger cycle disorders.
Polycystic ovary syndrome (PCOS) is one of the most common hormonal disorders and is typically associated with long, irregular or absent cycles. The cause is usually insulin resistance, which affects hormonal communication between the brain and ovaries and leads to elevated LH levels. As a result, follicles do not mature fully and ovulation often does not occur. In addition to cycle problems, other symptoms such as acne, hair loss, weight gain or elevated androgen levels are common. If you suspect PCOS may be behind your cycle problems, our PCOS self-test: Which PCOS type are you? can help you understand your situation better.
Hormonal contraceptives such as the pill, the contraceptive ring or hormonal IUDs affect natural hormone production. During use, there is no true cycle with ovulation. After stopping, the body often needs several months to find its own hormone regulation again. Common consequences are irregular cycles, intermenstrual bleeding, late ovulation or anovulatory phases. In some women, a “post‑pill syndrome” occurs, which shows up as long cycles or hormonal fluctuations.
Endometriosis, fibroids, adenomyosis and other gynecological conditions can cause cycle changes. Endometriosis is often associated with severe pain, long bleeding, intermenstrual bleeding and inflammation‑related hormonal changes. Fibroids can increase bleeding intensity and change the structure of the lining. Chronic inflammation in the pelvic area can also affect hormonal communication between the ovaries and the uterus.
A disrupted sleep‑wake rhythm affects the cycle directly. Shift work, jet lag or chronic sleep deprivation disrupt the circadian rhythm, which is closely linked to hormone production. Intense endurance or competitive sports can also dampen GnRH and LH release and lead to long or absent cycles. In such situations, the body prioritizes survival and saving energy over reproduction—especially when body fat levels are low.
In many cases, you can positively influence your cycle health—especially through lifestyle, diet, sleep and stress management. The menstrual cycle reacts sensitively to external and internal factors because hormonal processes are closely linked to energy, metabolism and mental well-being. With targeted, everyday measures, cycle length, ovulation stability and hormonal well-being can often be improved significantly.
A nutrient-dense, balanced diet supports hormone production, metabolism and energy availability—key building blocks of a healthy cycle. Omega‑3 fatty acids, vitamin D, B vitamins, magnesium and iron are especially important. Large calorie deficits, crash diets or irregular eating can slow follicle maturation or prevent ovulation. Stable energy intake and nutrient-rich meals, on the other hand, promote regular cycles and a balanced hormonal state.
Regular, moderate exercise has proven positive effects on cycle health, insulin sensitivity, stress processing and metabolism. Recommended activities include jogging, yoga, cycling, Pilates or strength training. Training that is too intense—especially with simultaneously low energy intake—can lead to missing ovulation. A balanced rhythm of activity and recovery is crucial to avoid hormonal stress.
Would you like to align your training optimally with your cycle to support a healthy cycle: Cycle‑based training
Chronic stress is one of the most common triggers of irregular cycles, PMS symptoms or delayed ovulation. Stress increases cortisol and can inhibit GnRH, LH and FSH release—hormones needed for ovulation. Relaxation techniques such as meditation, breathing exercises, yoga (hormone yoga), walks or journaling can help stabilize the nervous system. Mental load, emotional strain or persistent pressure can also impair cycle processes. Stress management is therefore a key lever for hormonal balance.
Restorative sleep is essential for hormonal stability. During sleep, the endocrine system regenerates and regulates important metabolic and stress hormones. Chronic sleep deprivation or shift work can disrupt LH and FSH release and thus impair ovulation and the luteal phase. A regular sleep schedule, ideal sleep duration (7–9 hours) and good sleep hygiene support cycle health sustainably.
Alcohol, excessive caffeine intake and high sugar consumption can influence hormonal balance. Alcohol can negatively affect liver metabolism and progesterone breakdown and may promote cycle disturbances. Caffeine can raise stress hormones in sensitive individuals and delay ovulation. High sugar and insulin spikes also affect androgen-related processes, which are particularly relevant in PCOS. A moderate, mindful approach helps reduce hormonal fluctuations.
Many small everyday habits can support hormonal balance: regular meals, breaks during the day, adequate hydration, daylight for your internal clock and gentle movement. Cycle-oriented planning—adapting strain and rest to the cycle phases—can also increase well-being. Being mindful of bodily signals promotes self-awareness and supports healthy cycle regulation in the long run.
There are many ways to observe your cycle—but not all are equally reliable. Some provide only rough estimates, while others make precise hormonal patterns visible. Especially for assessing cycle health, ovulation and hormonal disorders, choosing the right method is crucial. The following approaches show how different cycle monitoring can be—from simple calendar entries to medically recognized continuous temperature measurement.
Many women start with calendar apps or classic cycle calendars. These methods are based on the statistical assumption that a cycle follows a similar pattern each month. Apps often predict ovulation purely mathematically without incorporating real body data. This is particularly unreliable when cycles fluctuate, ovulation occurs late or hormonal disorders are present. Suitable for a rough orientation—but not precise enough for medical conclusions or when trying to conceive.
Bracelets and smartwatches often record parameters such as skin temperature, pulse or sleep phases. They provide a good overview of general health, but are not specifically designed for cycle diagnostics. Skin temperature shows hormonal changes only indirectly and reacts strongly to external factors such as room temperature, stress or movement. Wearables can therefore provide valuable lifestyle data, but no precise statement about whether and when ovulation occurred.
The NFP method combines classic basal body temperature and cervical mucus observation and can provide good insight into the cycle—provided it is performed correctly and consistently. However, the temperature method measures only once per day and is therefore susceptible to disruption: restless nights, alcohol, sleeping in or illness can distort the measurement result. NFP can confirm ovulation, but is less suitable for detecting complex cycle patterns, progesterone levels or subtle hormonal disorders.
For a medically sound assessment, it makes sense not only to estimate, but to really understand your cycle—including ovulation, the luteal phase and individual patterns.
The basal body temperature method provides only one data point per day and is therefore vulnerable to external influences. Continuous measurement, on the other hand, records core body temperature without interruption—an more direct and biologically more stable signal of hormonal changes. This makes it possible to identify ovulation, luteal phases and cycle patterns much more precisely. Especially with fluctuating cycles, PCOS or unclear symptoms, continuous measurement is the gold standard because it makes the true physiological dynamics visible.
OvulaRing measures core body temperature around the clock and makes hormonal processes visible that remain hidden with conventional methods. The technology provides precise information about ovulation, cycle length, luteal phase quality and hormonal irregularities. Healthcare professionals can use the data to identify disorders such as anovulation, progesterone deficiency, PCOS‑typical patterns or stress-related strain. For women who are trying to conceive, have unclear cycle disorders or want evidence-based cycle diagnostics, OvulaRing offers a medically sound basis that goes far beyond app estimates or manual temperature measurements.

OvulaRing enables a completely new form of cycle diagnostics because it measures core body temperature continuously—an even more precise and less disruption‑prone signal than basal body temperature. This makes hormonal processes visible that cannot be reliably captured with apps, wearables or NFP. OvulaRing provides medically evaluable data showing whether ovulation occurred, when it occurred and how stable the luteal phase was. This not only makes the cycle understandable, but also easier to interpret and assess in the long term.
Ovulation is the central event of every cycle—and OvulaRing makes it clearly identifiable. Continuous measurement records typical temperature patterns that correspond to the rise in progesterone after ovulation. These patterns are clearer, visible earlier and less prone to disruption than once‑daily basal temperature measurements. This means that even late, irregular or barely noticeable ovulation can be identified precisely, even in complex cycles.
We explain exactly how this works step by step at How OvulaRing works.
OvulaRing’s continuous temperature curves show more than just the timing of ovulation. They reveal typical patterns of the follicular phase, luteal phase and temperature stability. Findings such as flat curves, missing biphasic patterns, unstable luteal phases or continuously elevated temperatures can indicate hormonal disorders. Healthcare professionals can evaluate this data medically and identify cycle characteristics that are often missed with classic methods.
OvulaRing can make a wide range of cycle disorders visible, including missing ovulation (anovulation), delayed or atypical ovulation, progesterone deficiency, shortened luteal phases, PCOS‑typical patterns, stress-related strain or strongly fluctuating temperature patterns. This is especially helpful for women whose cycles appear “normal” externally but who still experience hormonal imbalances or symptoms. OvulaRing provides the clarity needed to address causes in a targeted way together with healthcare professionals.
Women with PCOS benefit particularly from continuous temperature measurement. Because PCOS often involves irregular or absent ovulation, temperature data helps distinguish real ovulatory events from hormonally driven “false ovulation” (e.g., LH peaks without ovulation). Longer or unclear cycles can also be interpreted better. OvulaRing makes it possible to confirm true ovulation, track the impact of lifestyle measures and visualize typical PCOS patterns that often go unnoticed with apps or classic temperature methods.
OvulaRing testimonials – getting pregnant despite PCOS
For women who are trying to conceive, OvulaRing offers particularly great benefits. Precise temperature curves show not only whether ovulation occurred, but also how stable the luteal phase was—an important factor for implantation. By determining the fertile window precisely, the chances of natural conception can be increased. At the same time, potential hurdles such as anovulatory cycles, progesterone deficiency or shortened luteal phases can be recognized early and supported medically. This gives you a reliable foundation for successful family planning.
The menstrual cycle can fluctuate naturally, but certain changes should be taken seriously. If cycle symptoms persist over several months or suddenly change significantly, a medical evaluation is advisable. Cycle health is a sensitive indicator of hormonal balance, metabolism and reproductive health. Medical advice helps identify causes in a targeted way and, if necessary, treat them early.
You should consider a gynecological check-up if one or more of the following signs occur:
Many cycle problems can be influenced through lifestyle, diet or stress management. Nevertheless, medical diagnostics are important if symptoms occur regularly or limit your quality of life. With modern cycle analysis, blood tests and ultrasound, a doctor can clarify hormonal imbalances, PCOS, endometriosis, thyroid changes or other causes. An early look at your cycle data—for example via continuous temperature measurement—provides valuable clues and makes medical assessment easier.
Many questions about cycle health relate to everyday uncertainty: What is normal? When should I worry? And which changes indicate that something is out of balance? The following frequently asked questions summarize the most important medical facts and help you understand your own cycle better.
A healthy cycle usually lasts 21 to 35 days and shows a clear biphasic pattern with ovulation and a luteal phase. What matters is not the exact length, but functionality: stable ovulation, sufficient progesterone production and a regular period that is neither too heavy nor too light are the key features. Every body has individual fluctuations—normal is what runs consistently and reproducibly.
A cycle is considered too long if it consistently lasts more than 35 days (oligomenorrhea) and too short if it regularly lasts under 21 days (polymenorrhea). Longer cycles often result from delayed or absent ovulation, while short cycles often point to a shortened follicular phase or a weak luteal phase. Sudden changes or persistent deviations should be evaluated medically.
Yes—stress is one of the most common causes of cycle changes. Cortisol, the stress hormone, can affect the release of GnRH, FSH and LH and thus change ovulation and cycle length. High mental load, lack of sleep or emotional strain often lead to long cycles, PMS symptoms or anovulatory cycles. Relaxation methods and a stable daily routine can help bring the cycle back into balance.
Ovulation can be identified most reliably via core body temperature—especially through continuous measurement. After ovulation, temperature rises measurably and stays elevated. Other methods such as observing cervical mucus, ovulation tests or apps can provide clues, but are less precise and more prone to disruption. Continuous temperature measurement provides objective data that makes ovulation timing and cycle patterns clearly identifiable.
The most effective measures to stabilize the cycle are: a nutrient-rich diet, enough sleep, moderate exercise, stress reduction, a stable daily routine and mindful use of caffeine, sugar and alcohol. Cycle monitoring helps make changes trackable and shows whether measures are working. If symptoms persist over months, medical evaluation is recommended.
Normal cycles have a clear structure: ovulation in the middle of the cycle, a stable luteal phase and regular bleeding. Abnormal are extreme fluctuations, recurring spotting, very heavy or very light bleeding, missing ovulation, constantly changing symptoms or severe pain. If you’re unsure whether your cycle patterns are within the normal range, cycle data and medical diagnostics can provide valuable clarity.
Cycle health is a crucial factor for hormonal well-being, quality of life and fertility. A regular, functional cycle with stable ovulation is a sign of a good interplay of hormones, metabolism and the nervous system. By better understanding your own cycles, practicing mindful self-care and using modern diagnostics, you can actively improve hormonal patterns—without striving for perfection, but with knowledge and clarity.
OvulaRing helps you understand your cycle objectively, identify ovulation with confidence and make hormonal patterns visible. This allows you to improve your cycle health in a targeted way and recognize changes early.
Wähle dein Ziel – wir zeigen dir die passenden nächsten Schritte.
You are currently viewing a placeholder content from Facebook. To access the actual content, click the button below. Please note that doing so will share data with third-party providers.
More InformationYou are currently viewing a placeholder content from Instagram. To access the actual content, click the button below. Please note that doing so will share data with third-party providers.
More InformationYou are currently viewing a placeholder content from Trustpilot. To access the actual content, click the button below. Please note that doing so will share data with third-party providers.
More InformationYou are currently viewing a placeholder content from X. To access the actual content, click the button below. Please note that doing so will share data with third-party providers.
More Information