
OvulaRing is covered by health insurance! Create your Cost estimate.
,You’ve been trying for quite some time to make your dream of Dream Child You know you should do it, but you just can’t seem to get it done?
Are you wondering if fertility treatment (IVF) is right for you?
We’ll show you how you can use OvulaRing to increase your chances of getting pregnant – more cost-effective, less stressful and more natural compared to IVF.
Here’s what you should know
One in six women becomes pregnant naturally after an unsuccessful IVF or ICSI treatment.
81% of women who are trying to conceive and who track their cycles closely become pregnant within 6 months.
The emotional strain of IVF is experienced as being just as distressing as the death of a family member.
Studies show a 52% rate of depression following IVF—regardless of whether the treatment was successful.
That’s what OvulaRing detects
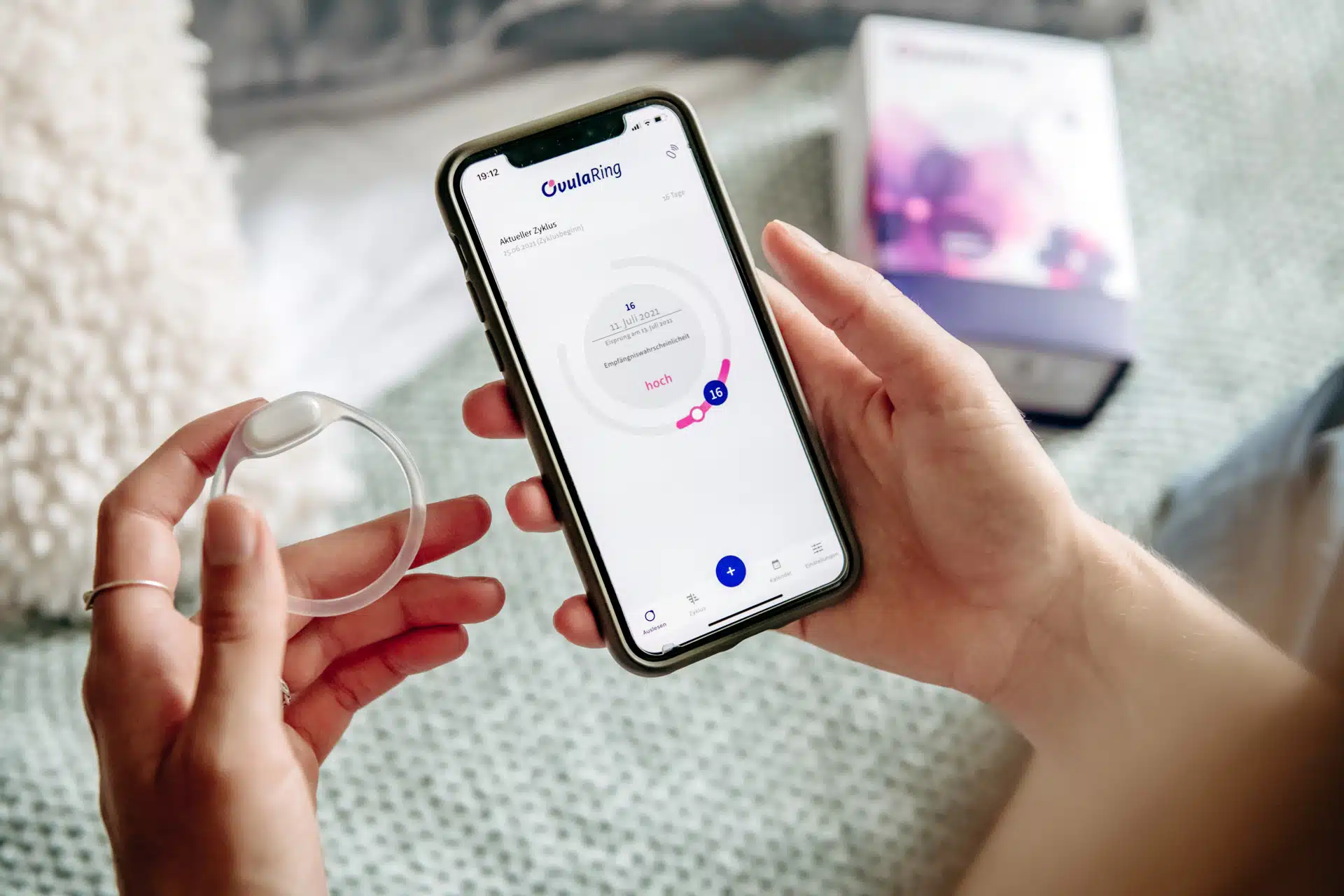
OvulaRing has been proven to prevent premature fertility treatment. It is medically tested, patented, and has been validated by multiple studies.
“OvulaRing can help prevent unnecessary IVF treatments.”

With OvulaRing On average, the users surveyed needed 4.4 months until the long-awaited pregnancy.
Those women who had already without OvulaRing who have tried to get pregnant have, on average 14.9 months tried.
The women surveyed who directly with OvulaRing have tried it have, on average, only 3.5 months needed to get pregnant.
On average, it took Women who at least 1.5 years tried unsuccessfully to get pregnant without the OvulaRing, and then with the OvulaRing an average of 6.3 months until the long-awaited pregnancy.
82% of women who OvulaRing: Pregnant were, required less than 6 months until pregnancy
97% were within 12 months pregnant.
And 99% were able to fulfill their dream of having a baby after 1.5 years of using OvulaRing.
As part of the OvulaRing Research Program for Women’s Health, OvulaRing users were surveyed at the time of their child’s birth. The women reported how long they had been trying to conceive before using OvulaRing and how long it took them to become pregnant while using OvulaRing.

Women who use OvulaRing are significantly more likely to achieve a desired pregnancy and give birth to a healthy baby than those who undergo IVF.
Source: IVF Yearbook 2020 & 2021, OvulaRing users, myovularing database.
Among 2,443 women with a confirmed desire to have children, there were 792 pregnancies and 92 miscarriages. This corresponds to a pregnancy rate of 32.4%. According to the IVF Yearbook, the pregnancy rate was 27.8%. Of all women treated with IVF, only 20% had a live birth, whereas 28.7% of OvulaRing users had a live birth.

OvulaRing is a patented method for cycle and fertility monitoring. OvulaRing is a biosensor that measures core body temperature at 288 measurement points per day. This makes it possible to to track the entire menstrual cycle. This allows the user’s fertile window to be determined with great precision. The recorded data is analyzed using algorithms and is immediately available to the user and her healthcare providers. This makes it possible to monitor both the pre-cycle and the treatment cycle with minimal effort.
For same-sex couples and singles hoping to have children, timing is crucial when it comes to conception. One method of artificial insemination used to achieve pregnancy is the so-called Heiminsemination. In this method, the donor’s sperm is inserted into the vagina using a needle-free syringe. However, the method can only be successful if the woman keeps a very close eye on her ovulation date. With OvulaRing, couples and singles can perform insemination entirely without medical assistance in a private setting. By precisely determining and predicting fertile days with OvulaRing, it is possible to coordinate home insemination appointments with the donor and incorporate them into daily life.
In natural-cycle IVF, the eggs are not stimulated. Fertilization takes place during natural ovulation. In natural-cycle IVF, it is possible to use the OvulaRing to personalized stimulation therapy and to determine the optimal time for egg retrieval much more easily and accurately. This approach takes into account not only the current cycle but also the woman’s individual cycle biology, based on her previous cycles. This information is used to tailor treatment to the individual. All of this leads to more effective treatment while reducing costs and side effects. Here you can find more information about IVF in a natural cycle
Yes, many women conceive naturally after an unsuccessful IVF or ICSI cycle. Studies show that about one in six women who undergo assisted reproduction later conceive spontaneously. And with OvulaRing, you can pinpoint your fertile days and significantly increase your chances of a natural pregnancy—without any hormones or invasive procedures.
In addition to IVF, there are various natural methods that can help you conceive. These include cycle tracking, close monitoring of ovulation, dietary changes, and medically approved aids such as the OvulaRing. This patented cycle tracker measures your basal body temperature around the clock and identifies your fertile window. This allows you to increase your chances of getting pregnant without the need for hormone therapy.
The term “natural conception” refers to conception that occurs without artificial insemination in a laboratory. Unlike with IVF or ICSI, fertilization of the egg takes place inside the woman’s body. OvulaRing supports this natural process by determining the exact time of ovulation, thereby increasing the likelihood of successful fertilization.
Yes, it is certainly possible to conceive naturally after ICSI. Some women report that, following an unsuccessful ICSI cycle, they were eventually able to get pregnant with the help of cycle tracking tools like OvulaRing. By accurately identifying ovulation, you can make the most of your fertile days and increase your chances of a natural pregnancy.
OvulaRing analyzes your entire cycle 288 times a day and provides a uniquely accurate picture of your fertility. On average, users become pregnant after just 4.4 months—significantly faster than with traditional methods or IVF. The ring is medically tested, covered by health insurance, and can help avoid unnecessary fertility treatments.
Despite endometriosis, unsuccessful IVF attempts, and having only one fallopian tube, she got pregnant using the OvulaRing: "But with the ring, I could tell right away that my body was doing everything right! That really restored my confidence in my body."
Lisa's Testimonial

"Since I had done everything in my power to avoid getting pregnant over the past 15 years, it never even crossed my mind that getting pregnant might be even remotely complicated. However, I was quickly proven wrong. After unsuccessful IVF, I got pregnant naturally."

"After two years of trying unsuccessfully to conceive, visits to the fertility clinic, and three rounds of artificial insemination, I was finally pregnant. I've never tried a more convenient way to track my cycle. This ring is an absolute game-changer for all women!"


Join our newsletter and get your 10% discount for your starter package. Enter your email to continue.
You are currently viewing a placeholder content from Facebook. To access the actual content, click the button below. Please note that doing so will share data with third-party providers.
More InformationYou are currently viewing a placeholder content from Instagram. To access the actual content, click the button below. Please note that doing so will share data with third-party providers.
More InformationYou are currently viewing a placeholder content from Newsletter2Go. To access the actual content, click the button below. Please note that doing so will share data with third-party providers.
More InformationYou are currently viewing a placeholder content from Trustpilot. To access the actual content, click the button below. Please note that doing so will share data with third-party providers.
More InformationYou are currently viewing a placeholder content from X. To access the actual content, click the button below. Please note that doing so will share data with third-party providers.
More Information